Why Timing Is Suddenly the Main Character
It’s 11:30 p.m.
Your athlete has just finished a hard evening session, scrolls on their phone in bed with the lights on, answers a few work emails, grabs a late snack, and finally falls asleep after midnight.
Calories? Reasonable. Training volume? On point.
Yet their blood pressure is creeping up, their fasting glucose looks a bit worse each year, and recovery feels… stuck.
We tend to blame the usual suspects stress, age, travel, genetics. A new scientific statement from the American Heart Association (AHA) adds a sharper lens: maybe the real issue is that their entire day is out of sync with their body clock.
This statement, published in Circulation in October 2025, isn’t about one more biomarker or one more drug. It’s about circadian health how well our internal clocks line up with the outside world and how that alignment (or misalignment) shapes cardiometabolic risk.
For GPNi® coaches, athletes, and practitioners, this isn’t just “sleep hygiene 2.0”. It’s a shift in how we think about training, nutrition, and recovery timing as part of heart and metabolic health.
What the AHA Means by “Circadian Health”
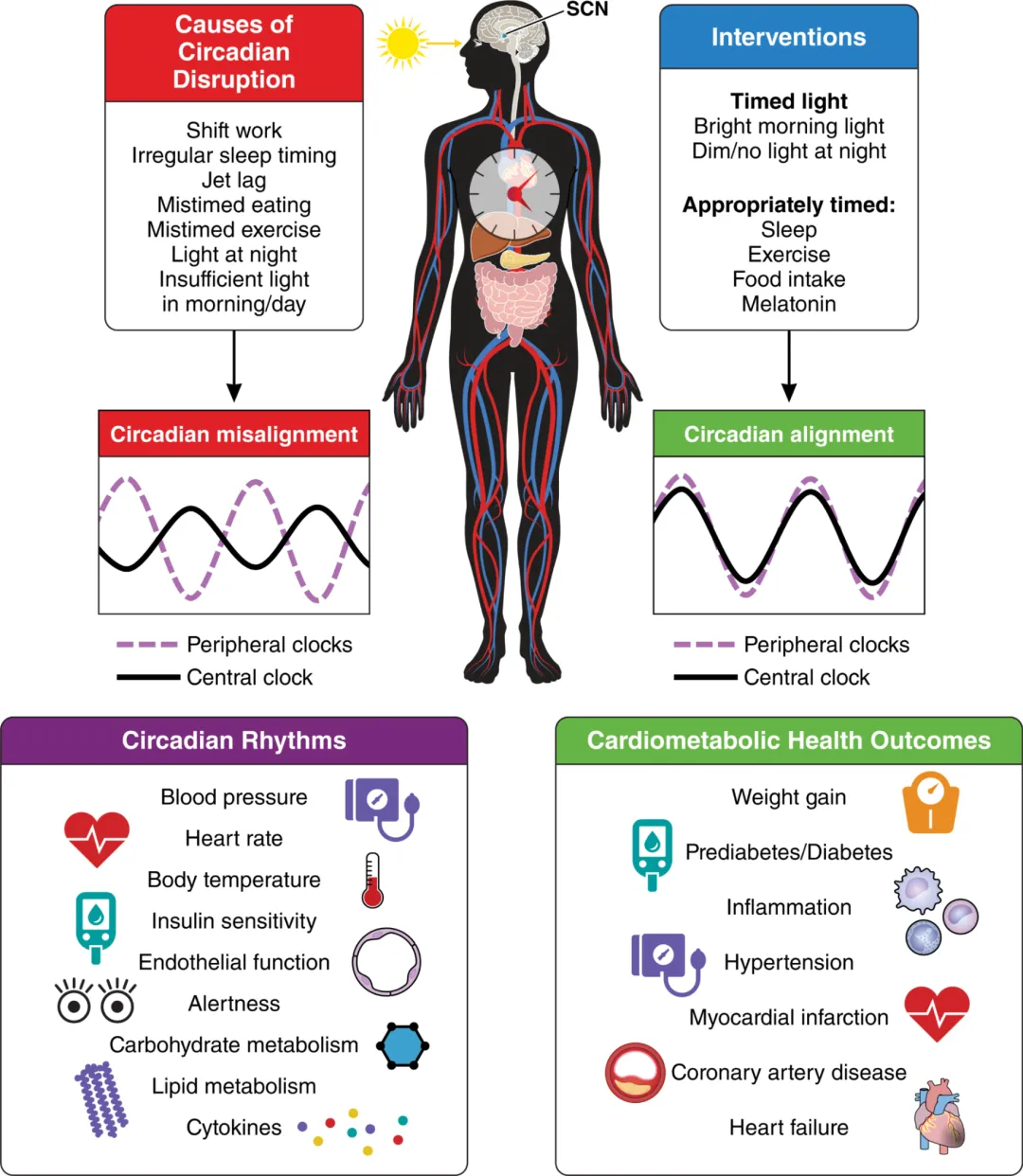
The AHA statement starts with a simple idea:
We all run on a network of body clocks a central clock in the brain and many peripheral clocks in organs like the heart, liver, muscle, and fat tissue.
These clocks create ~24-hour rhythms in heart rate, blood pressure, hormones, glucose handling, and more.
“Circadian health” is their term for when:
- those internal rhythms are strong and regular, and
- they are aligned with the external light-dark cycle.
In plain language: your body expects light in the morning, movement and meals mostly in the daytime, and darkness plus sleep at night. The more consistently you line up with that pattern, the easier it is for your heart and metabolism to do their job.
The problem? Modern life often pulls us in the opposite direction:
- Rotating or night shift work
- Late-night screens and bright indoor lighting
- Irregular bedtimes and “social jetlag”
- Late eating and “second dinners”
- Intense training sessions close to midnight
The AHA’s review links this kind of circadian disruption with a higher risk of obesity, type 2 diabetes, hypertension, and cardiovascular disease.
Four Levers That Move Your Body Clock

The statement highlights four behavioural “time cues” that can either synchronize or scramble your circadian system: light, sleep, meals, and movement.
Let’s unpack those through a GPNi® lens.
1. Light: The Main Dial
Light is the primary external signal for the central clock in the brain. Morning light helps anchor your rhythm; bright light at night can push it later.
The AHA statement notes that:
- Morning bright light supports healthy circadian timing.
- Night-time light exposure, especially blue-rich light from screens and overhead LEDs, can suppress melatonin, shift sleep later, and disturb blood pressure and metabolic regulation.
From a practical perspective, this means:
- Get outside or near a bright window in the first 1–2 hours after waking.
- In the last 1–2 hours before bed, dim the room, reduce screen brightness, or use warmer light settings.
- Athletes who train indoors all day may actually need intentional morning light exposure just as much as a good warm-up.
2. Sleep: Not Only “How Much” but “How Regular”

The AHA highlights something many athletes intuit but rarely measure:
It’s not just sleep duration that matters sleep timing and regularity strongly relate to obesity, type 2 diabetes, and cardiovascular risk.
Across several cohorts, people whose bedtimes and wake times drift a lot from day to day show higher rates of obesity, diabetes, and CVD, even when total sleep time isn’t dramatically different.
For GPNi® practitioners, a simple rule of thumb is:
“Pick a 60–90 minute window for bedtime and wake time, and stick to it most days even on ‘off’ days.”
For competitive athletes, this can be surprisingly hard once late-night games, travel, and media obligations are involved. That’s exactly where planning and sometimes negotiation with teams or employers comes in.
3. Meals: When You Eat Shapes Risk, Not Just What
One of the clearer messages from the AHA statement is that late eating isn’t neutral.
The authors note that:
- Eating a larger share of daily calories later in the day, especially after ~21:00, is associated with higher risk of type 2 diabetes, hypertension, and CVD, even after accounting for total calorie intake.
- Irregular meal timing can also disturb metabolic rhythms.
So yes, macros and fibre still matter but timing is its own variable now.
A GPNi®-style approach could look like this for most non-shift-working adults:
- Let breakfast and lunch carry a solid portion of your daily calories and carbs.
- Keep the evening meal lighter and earlier when possible.
- Avoid routine “second dinners” or heavy snacks in the 1-2 hours right before bed.
We don’t need perfection here. Even nudging the largest meal from 22:00 back to 19:30, most days, is a meaningful change for your body clock.
4. Physical Activity: Exercise as a Secondary Time Cue
Exercise doesn’t dominate the circadian system the way light does, but it still acts as a secondary synchronizer.
The AHA statement points to emerging evidence that:
- Morning or afternoon activity can advance circadian phase in some people (helping earlier sleep timing).
- Vigorous evening exercise may delay the clock for some individuals and, if too close to bedtime, can disturb sleep onset.
This doesn’t mean “never train at night” many sports simply don’t have that luxury. But if someone:
- trains late,
- then gets strong light exposure from screens,
- then eats a large meal,
- then sleeps short and irregular hours,
The stack of circadian stressors becomes pretty obvious. At GPNi®, we increasingly treat training timing as part of the health discussion, not just a logistics question.
What This Means in Practice for GPNi® Coaches and Students

The AHA statement is written for cardiologists, epidemiologists, and policy makers but the practical levers land squarely in our world: daily behavior, training, and nutrition.
Here’s how we’d translate it into everyday coaching language:
1. For the General Public and Recreational Trainees
If someone is mostly healthy but worried about long-term heart and metabolic risk, we’d frame circadian health as “tidying up the rhythm of the day”:
- Light
- Sleep
- Meals
- Movement
2. For Shift Workers, Night Owls, and Frequent Travelers
The AHA statement is explicit: rotating and night shift work is a major driver of circadian disruption, with higher rates of obesity, diabetes, hypertension, and CVD.
From a GPNi® perspective, we don’t get to magically “fix” shift schedules. But we can help people:
- Reduce unnecessary extra disruption (for instance, not flipping back and forth between day- and night-type schedules on days off).
- Use targeted light exposure (brighter light during intended “day,” darker environment before sleep, even if that’s 09:00).
- Keep meals in a consistent window relative to their main sleep period, rather than snacking through the entire night.
3. For Performance-Oriented Athletes
Most high-level athletes already know sleep affects performance. What’s newer is the appreciation that when they sleep, eat, and train can shape:
- Long-term blood pressure and vascular health
- How their body handles glucose and lipids
- Injury recovery and tissue repair rhythms
For this group, GPNi®-aligned priorities could be:
- Protecting a stable sleep wake schedule even in the off-season, rather than bouncing between “night owl in off-season” and “disciplined schedule in-season”.
- Building training plans that cluster the hardest work earlier in the day when possible.
- Matching carbohydrate timing to daytime training and competition, not to late-night boredom eating.
A Simple Way to Frame This for Clients

When you strip away the technical language, the AHA message fits into one short idea we use a lot at GPNi®:
“Your heart doesn’t just care what you do. It cares when you do it, and how predictable that pattern is.”
We won’t get every athlete or client to a perfect “textbook” schedule. Life, work, travel and competition will always add noise. But if we can:
- get them more light in the morning,
- less light and food late at night,
- more regular sleep timing, and
- training that mostly lives in the biological “day”
we’re not just helping them perform tomorrow.
We’re quietly taking pressure off their arteries, pancreas, and heart for the decades ahead.
From GPNi®’s perspective, that’s exactly where sports nutrition and performance coaching should sit: between today’s performance and tomorrow’s health, using science like this AHA statement as our compass.
References
- Knutson KL, Dixon DD, Grandner MA, et al. Role of circadian health in cardiometabolic health and disease risk: a scientific statement from the American Heart Association. Circulation. Published online October 28, 2025. doi:10.1161/CIR.0000000000001388.
- American Heart Association. Top Things to Know: Role of Circadian Health in Cardiometabolic Health & Disease Risk. 2025.
- American Heart Association News. Study finds disruptions to circadian rhythm increase risk of heart disease, other conditions. October 28, 2025.
- CardioCare Today. AHA statement emphasizes link between circadian rhythm, cardiometabolic health 2025.